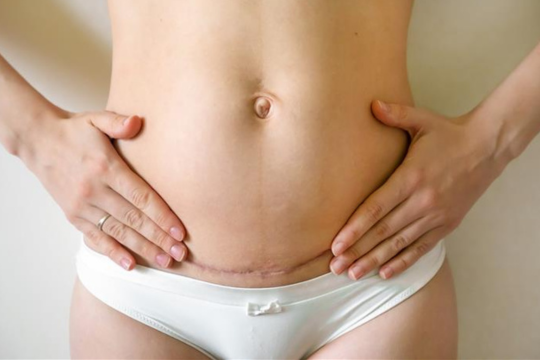
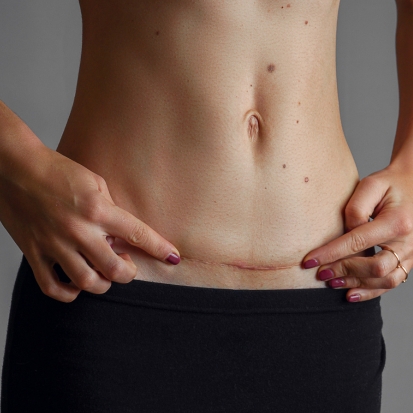
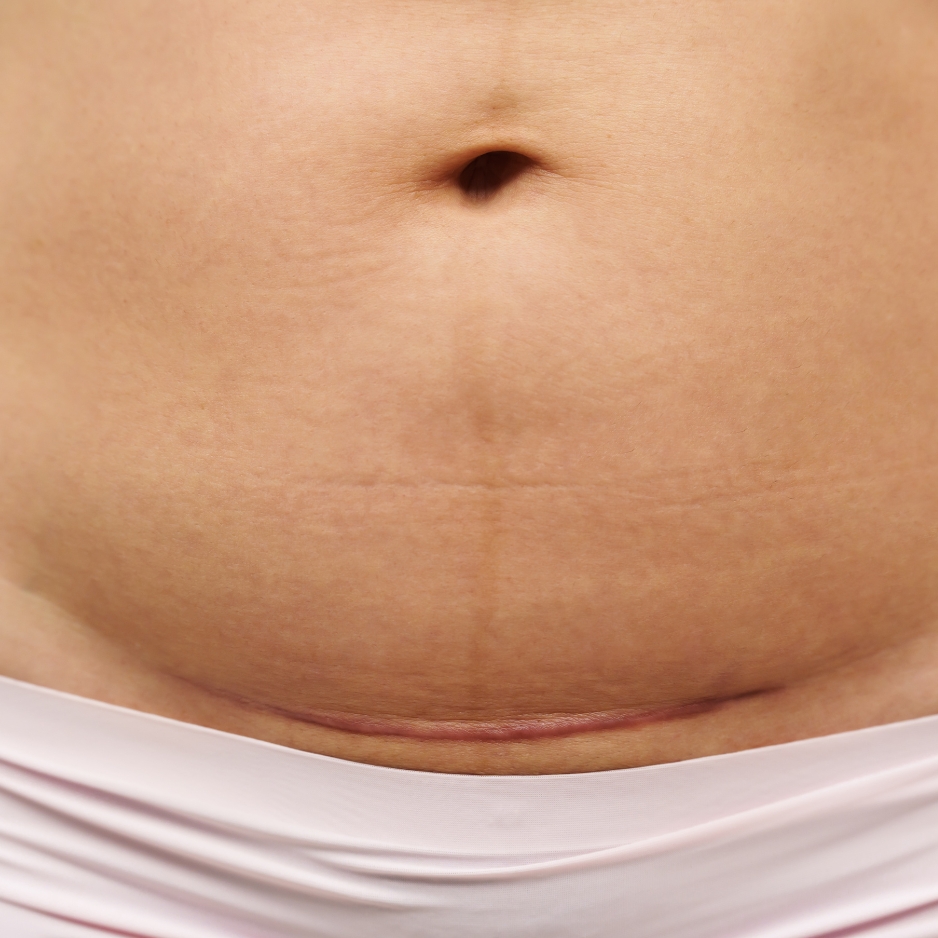
Dealing with an older C-section scar that’s red and smells

If your old C-section scar has become red and smelly, it’s understandable to feel concerned. A well-healed C-section scar should not have a strong odour or ongoing redness. If these symptoms appear months or even years later, they could indicate an underlying issue.
Understanding the possible causes and solutions can help you take the right steps for scar treatment.
Common causes of redness and odour in old C-section scars
Here are some common reasons why an old C-section scar may develop redness and an odour.
Infection
Even long after surgery, a C-section scar can become infected—especially if moisture or bacteria build up in skin folds. A bad smell, especially a unpleasant odour, can be a sign of a low-grade infection or bacterial overgrowth in the skin folds around the scar. Signs of infection may include:
- Increased redness and swelling.
- A foul-smelling discharge.
- Pain or tenderness around the scar.
- Fever or chills in severe cases.


If you notice your C-section scar is red and weeping, consult your doctor immediately. Antibiotics or topical treatments may be needed.
Research on scar management highlights the importance of recognising infection early to prevent complications. According to Meaume et al. (2014):
“Persistent redness, swelling, and the presence of purulent exudate are indicators of infection in scar tissue. Left untreated, these infections can contribute to prolonged inflammation, hypertrophic scar formation, and even delayed wound healing.”
Trapped moisture and poor ventilation
Moisture buildup can lead to skin irritation and bacterial growth, particularly if your scar sits within a skin fold. A C-section wound that smells but isn’t open may simply need better care and ventilation (Hoeksema, 2018). Prevent this by:
- Keeping the area dry and clean.
- Using absorbent powders to reduce moisture.
- Wearing loose, breathable clothing.
Skin irritation and scar changes
An older scar can become red, itchy, or raised over time. This might be due to hypertrophic scarring, keloids, increased skin sensitivity, or irritation from clothing, friction, and skincare products.
Possible triggers:
- Allergic reactions to fabrics or skincare products.
- Constant friction from tight clothing.
- Hormonal changes affecting skin texture.
Applying a silicone scar sheet such as Scarban C-Section can help protect and soften the scar.
How to treat and prevent issues with your old C-section scar?
If your C-section wound is open, painful, or smelly, seek medical help immediately. For minor symptoms, try the following:
-
Improve hygiene: Wash the area daily with a mild soap and ensure it’s completely dry before dressing or applying silicone scar sheet.
-
Use silicone therapy: C-Section silicone sheets help protect and improve scar appearance.
-
Manage irritation: A moisturizing cream can be safely used in combination with a silicone sheet. Learn how to combine both products in the blog: The benefits of ALHYDRAN and Scarban for C-Section Recovery.
When to see a healthcare professional?
Seek medical advice if:
- Your C-section scar is red after three months or more and not improving.
- You notice red spots around the C-section scar that spread.
- There is pus, foul-smelling discharge, or pain.
- Your C-section scar is still red after a year.
A scar should heal completely within six to twelve months, so persistent symptoms should not be ignored (Mustoe et al., 2002).
Personal experiences and community advice
Many people turn to online forums and support groups, such as Mumsnet.com, when dealing with C-section scar issues. Here are some real experiences from individuals who have faced similar challenges:
Recurrent Infections
One mother shared her struggle with a persistent infection that required multiple courses of antibiotics over several weeks. Despite the challenges, she emphasized the importance of advocating for oneself and seeking continuous medical attention until the infection was fully resolved.
Managing Overhang and Moisture
Another individual discussed the difficulties of keeping the C-section area dry, especially with an overhang. She found that using sanitary pads to absorb moisture and keeping the area clean helped in the healing process.
Itchiness and Numbness
A woman recounted that even six months post-surgery, her scar remained itchy and areas around it were numb. She learned that this is a common experience and that sensations often return over time.
Would you like to share your own experience? Let us know in the comments.
Final thoughts
An old C-section scar turning red or smelly can be a sign of infection, irritation, or changes in scar tissue. Keeping the area clean, using silicone therapy, and seeking medical help if symptoms persist can ensure your scar stays healthy.
If you’re looking for effective scar management, using Scarban C-Section silicone sheets can help reduce redness, irritation, and scar thickness, supporting a smoother recovery.
Would you like to learn more about C-section scar recovery? Browse our website for expert advice, real stories on C-section scar healing or more helpful articles.
References
-
Anthonissen, M., Daly, D., Janssen, P., & Van den Kerckhove, E. (2016). The effects of conservative treatments on burn scars: A systematic review. Burns, 42(3), 459-469.
-
Hoeksema, H. (2018). Scar management by means of occlusion. Journal of Wound Care, 27(6), 368-375.
-
Meaume, S., Le Pillouer-Prost, A., Richert, B., Roseeuw, D., & Vadoud, J. (2014). Management of scars: Updated practical guidelines and use of silicones. European Journal of Dermatology, 24(4), 435-443.
-
Monstrey, S., & Middelkoop, E. (2014). Updated scar management practical guidelines: Non-invasive and invasive measures. Journal of Plastic, Reconstructive & Aesthetic Surgery, 67(8), 1017-1025.
-
Mustoe, T. A., Cooter, R. D., Gold, M. H., Hobbs, F. D. R., Ramelet, A. A., Shakespeare, P. G., ... & Ziegler, U. E. (2002). International clinical recommendations on scar management. Plastic and Reconstructive Surgery, 110(2), 560-571.
-
Niessen, F. B., Spauwen, P. H. M., Schalkwijk, J., & Kon, M. (2016). Topical silicone sheet application in the treatment of hypertrophic scars and keloids. Journal of Clinical and Aesthetic Dermatology, 9(10), 28-35.
-
Wang, F., Li, X., Wang, X., & Jiang, X. (2020). Efficacy of topical silicone gel in scar management: A systematic review and meta-analysis of randomised controlled trials. International Wound Journal, 17(5), 1165-1175.
About the Author

Categories